| An established treatment for Parkinson's disease involves implanting electrodes in the brain and connecting them to a pacemaker.
by Katherine Nightingale
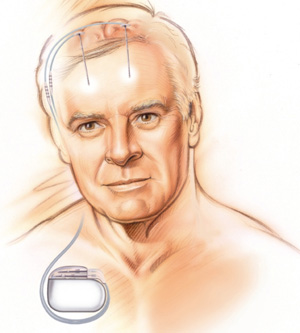 Photo courtesy
of Medtronic, Inc
Photo courtesy
of Medtronic, Inc
Deep Brain
Stimulation involves electrodes implanted in the brain connected
to a pacemaker.
|
|
Mike Robins was diagnosed with Parkinson's
disease 13 years ago. A successful businessman, his life was drastically
changed when he had to deal with the constant tremors caused by
the disease. Seven years ago, he was proposed a new treatment involving
brain surgery called Deep Brain Stimulation (DBS) and was one of
the first people in the world to undergo this procedure. It was
successful and all the symptoms of the disease were eradicated.
Today about 40,000 people have received DBS and although there is
serious surgery involved, the positive results have encouraged researchers
to look into how it could be used to treat other neurological diseases.
DBS involves implanting one (or in some cases two) electrodes in certain areas of the brain. These are attached by wires to a pacemaker just under the collarbone. The pacemaker controls the strength and rate of high-frequency electrical impulses that are sent up wires embedded in the neck to the electrodes. The impulses either completely stop or severely reduce the activity in the area of the brain where the electrodes are located.
The effects of DBS can be dramatically displayed by watching Robins operate his pacemaker. It can be turned on and off almost magically by holding a magnet against the area of the chest where it is implanted. When Robins turns off his pacemaker he begins to shake and shudder down the right-hand side of his body. His speech becomes laboured and he is clearly stressed as he puts considerable effort in continuing to pace the room as he did with such ease a few moments ago. Bringing the magnet to his chest again, his body relaxes and his breathing returns to a normal rate as his pacemaker is reactivated.
 Photo
courtesy of Medtronic, Inc
Photo
courtesy of Medtronic, Inc
Brain pacemaker:
Similar to a cardiac pacemaker, this one sends electrical
impulses to electrodes in the brain.
|
In the case of Parkinson's disease,
DBS stops the overactivity that causes muscle tremors and stiffness
of limbs. These symptoms are caused by a lack of the neurotransmitter
dopamine in the brain. Cells of the substantia nigra - an
area of the brain just above the brain stem - normally make dopamine
but Parkinson's causes these cells to die, resulting in a lack of
dopamine. Since dopamine helps to regulate areas of the brain that
control movement, like the thalamus, subthalamic nucleus
and the globus pallidus, a lack of it causes some of these
areas to go into overdrive. By targeting these areas, DBS can block
the unwanted nerve traffic.
It may sound like a miracle treatment, but DBS does involve major surgery. Most seriously, any brain surgery carries a risk of cerebral haemorrhage - bleeding on the brain - and the impairment of other brain functions like speech and vision. With DBS surgery, there is the added possibility of the implant dislodging or becoming infected, the patient simply not responding to the treatment and the need to undergo further surgery to replace the pacemaker about every four years when the battery runs out.
In terms of post-operative care, it can sometimes be hard to find an electrical impulse with the right frequency and voltage for the patient. And although DBS may permanently remove the symptoms of Parkinson's, it also ties the patient to permanent aftercare.
There are other options for Parkinson's sufferers but these also have their drawbacks. Lesional surgery, in which the overactive areas of the brain are burned or cut, cannot be used for all patients since some areas of the brain are too sensitive to be treated in this manner. Drugs, many of which mimic the effects of dopamine, can also be used and are a successful treatment for some patients, though they can lose their effectiveness over time. Some patients suffer side effects from drugs such as involuntary movements, nausea, hallucinations and irregular heartbeat depending on the class of drug being taken. About one in five patients do not respond to drugs at all, and these are the patients most likely to be considered for DBS.
 Photo
courtesy of Bill Innanen
Photo
courtesy of Bill Innanen
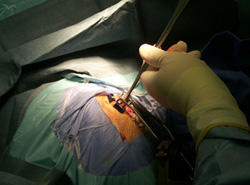
In the operating
room: DBS involves major brain surgery.
|
It's not only Parkinson's sufferers that are being offered this treatment. DBS is already being used routinely to treat other neurological movement disorders like dystonia, which results in involuntary spasms, and Essential Tremor, an extreme version of the ordinary trembling we all experience in certain situations. Researchers are also considering DBS as a way to treat epilepsy, Tourette syndrome and depression. The lifting of depression is a side effect of DBS for some Parkinson's patients and there has been a small but striking study showing that the electrical stimulation of a small area of the frontal cortex can alleviate depression in patients that don't respond to anti-depressant medication. When the electrode carrying the electrical impulses hits the right spot, some patients have likened it to "a black cloud lifting."
At the end of the day, we must remember
that DBS is a treatment and not a cure. For people like Mike Robins,
it has helped him lead a more normal life, but it may not work for
everyone and not everyone may be willing to take the risks involved.
For less severe conditions perhaps DBS is not the way forward but
for many it is one of the only options if they want to feel comfortable
in their own bodies again.
For more info:
National Institute of Neurological Disorders and Stroke
http://www.ninds.nih.gov/disorders/deep_brain_stimulation/deep_brain_stimulation.htm
Bill Innanen's DBS surgery at John Hopkin's Hospital
http://mac2.innanen.com/~bill/parkinsons/DBSsurgery/
|
